Malawi’s ban on dual practice divides health sector
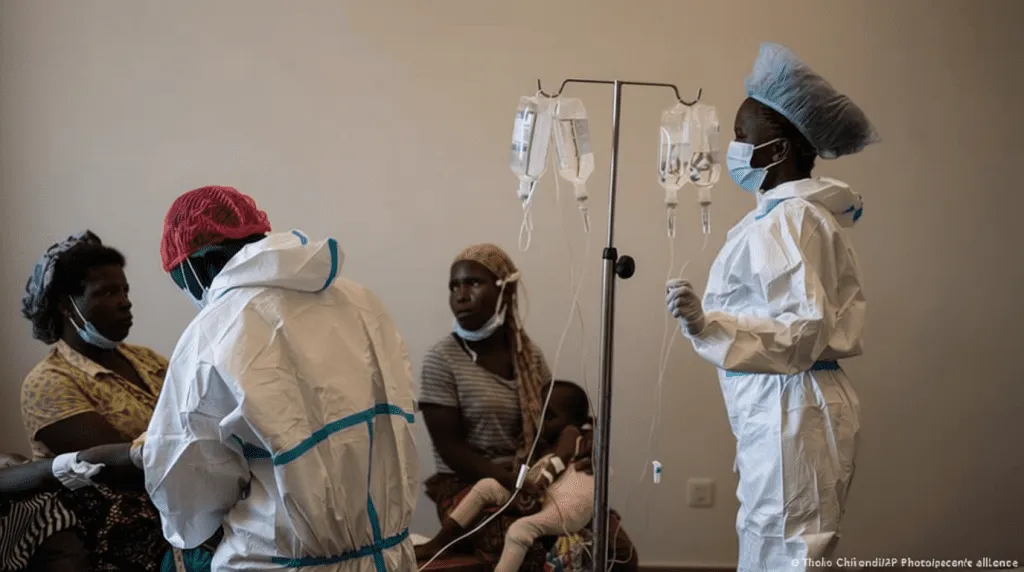
Malawi’s ban on dual practice divides health sector
Malawi recently enacted a regulation prohibiting public health workers from holding private medical positions. The government asserts the policy addresses corruption, yet medical professionals express concern it might worsen staffing deficits. The directive mandates that all public sector doctors and nurses must cease working in private clinics, hospitals, pharmacies, or diagnostic centers while employed by the state. Additionally, any worker who owns or partially owns a private facility is required to relinquish their stake within 30 days or risk dismissal and legal consequences.
Investigation Sparks Policy Change
The rule was triggered by an investigative report from the Nyasa Times, which exposed a widespread corruption network in several public hospitals. Patients were often compelled to pay illicit fees for services intended to be free, with security guards, clerks, nurses, and clinicians collaborating in bribery schemes. Those who paid could bypass queues, while others endured delays or received no care. The study highlighted how access to treatment had effectively become a cash-based privilege, disadvantaging low-income individuals.
Malawi’s president, Peter Mutharika, defended the ban as a necessary step to combat corruption. He cited instances where staff demanded unofficial payments, redirected patients to private clinics, and diverted medications from public hospitals for resale in their own pharmacies. Reports also revealed that many health workers frequently arrived late or left early to attend to private patients, creating critical service gaps in already overburdened facilities.
Controversy Over Rights and Innovation
“I think the directive has no basis,” said Maziko Matemba, executive director of the Health and Rights Education Program. “It is illegal and an infringement of human rights.”
Health experts argue the policy undermines workers’ economic rights, as public sector wages remain insufficient. Doctors and nurses contend that private practice is their only means to cover financial needs, and some fear the measure could push them to abandon public service altogether. Matemba also warned that the policy might stifle medical innovation, noting that private clinics often drive advancements in health services.
The Society of Medical Doctors in Malawi has initiated legal action, claiming the directive is overly strict and threatens the stability of the national health system. Solomon Chomba, leader of the Human Resource for Health Coalition, criticized the approach as “wrong,” emphasizing its impact on workers’ livelihoods. Dr. Victor Mithi, president of the society, highlighted risks of brain drain, with critical expertise potentially leaving the public sector.
Supporters See Benefits
Despite the backlash, supporters of the ban argue it is a vital step toward curbing corruption and upholding ethical standards. The Malawi Health Equity Network praised the measure as a “long-overdue intervention” to combat illegal fees, coercion, and unequal access to care. Some residents interviewed by DW also endorsed the decision, noting that public hospitals often lacked basic supplies, forcing patients to seek care from privately owned pharmacies.
